By Esther Ososanya
Unregulated access to Ampiclox and emergency contraceptives is fuelling fertility fears, misinformation, and rising drug resistance, experts warn.
In Nigeria’s bustling pharmacies and corner shops, a troubling trend has taken root. Women are increasingly relying on antibiotics like Ampiclox and Ampicillin not to fight infections but as makeshift contraceptives.
At the same time, emergency contraceptive pills are being used regularly and often without medical supervision. The consequences, experts warn, are deeply disturbing: reduced contraceptive efficacy, delayed fertility, and a silent surge in antibiotic resistance that could cripple the country’s health system.
According to Dr Opiti Chukwuneku, Associate Director-Technical at USAID’s ACE3 Project and a specialist with Health System Consult Limited, while early studies once hinted at links between antibiotics like Ampiclox and contraceptive failure, contemporary research shows that these antibiotics do not directly reduce the effectiveness of hormonal contraceptives.
“These antibiotics may interfere with oral contraceptives indirectly,” Dr Chukwuneku explains. “If a woman vomits or experiences severe diarrhoea after taking a contraceptive pill, the medication may not be fully absorbed. This reduces its efficacy and increases the risk of unintended pregnancy.”
To err on the side of caution, he recommends that women use a backup contraceptive method like condoms while on antibiotics and continue for at least seven days after completing the drug course, especially if gastrointestinal symptoms occur.
NO, AMPICLOX DOES NOT PREVENT PREGNANCY
The dangerous belief that antibiotics like Ampiclox can serve as birth control is not only medically baseless but also deadly. Dr Chukwuneku clarifies that the repeated misuse of antibiotics, particularly without treating underlying infections, can contribute indirectly to infertility.
In women, poorly treated sexually transmitted infections (STIs) may evolve into pelvic inflammatory disease (PID), which can scar the fallopian tubes and compromise fertility. In men, untreated infections can damage reproductive function as well.
The doctor is quick to debunk a prevailing myth: “Hormonal contraceptives, whether pills, injections, or implants, do not cause long-term infertility. They may temporarily delay ovulation, but once discontinued, the body resumes its normal rhythm, usually within weeks to a few months.”
Still, he notes, many women wrongly blame contraceptives for infertility when pre-existing conditions like PCOS or irregular periods reappear after stopping the pill.
THE EMERGENCY DRUG THAT’S BECOME A LIFESTYLE
Emergency contraceptives designed for rare, urgent use have become routine for many Nigerian women. Dr Chukwuneku warns that overreliance on these high-dose hormone pills is risky.
Frequent use can cause irregular menstruation, spotting, unpredictable ovulation, and ultimately reduced contraceptive efficacy.
“This is the most significant long-term effect of misuse, not infertility, but a much higher likelihood of unintended pregnancies,” he says.
Economically, the costs stack up. Emergency contraceptive pills are more expensive per dose than regular methods, making habitual use a financial burden, particularly for low-income women.
“Women who find themselves frequently needing emergency contraception should be counselled and provided with regular, more effective options – IUDs, implants, or oral pills – not left to navigate alone,” he adds.
THE RESISTANCE CRISIS: ANTIBIOTICS MISUSED AND DANGEROUSLY ACCESSIBLE
Beyond reproductive health, the widespread misuse of antibiotics like Ampiclox is feeding a public health nightmare: antimicrobial resistance (AMR).
“This crisis is being driven by unrestricted access,” Dr Chukwuneku explains. “In Nigeria, antibiotics are widely sold over the counter – no prescriptions, no guidelines, no warnings. People are even taking them to prevent pregnancy, which they absolutely do not do.”
The consequence? Bacteria are evolving. Once-treatable infections are becoming stubborn killers. Healthcare costs are rising. And the drugs we’ve long relied on may soon become useless.
READ ALSO: “Wounds from Within: When Pads Hurt More Than Periods”
To curb the rising threat, Dr Chukwuneku recommends a total ban on over-the-counter sales of antibiotics.
Chukwuneku recommended that regulatory bodies like NAFDAC and the Pharmacists Council of Nigeria (PCN) must scale up surveillance, introduce strict penalties for violators, and explore tech-based solutions like electronic prescription tracking.
He also calls for a nationwide surveillance system led by the Nigeria Centre for Disease Control and Prevention (NCDC) to monitor antibiotic usage and resistance trends, especially from private and public healthcare providers.
Also speaking in an exclusive interview with Pinnacle Daily, Dr Izuagba Kelechi of the Medical Women’s Association of Nigeria (MWAN-FCT) warned that this dangerous practice could lead to infertility, hormonal imbalances, and antibiotic resistance.
She emphasised that most antibiotics don’t interfere with birth control pills, except for specific drugs like rifampicin. However, antibiotic side effects such as vomiting and diarrhoea can reduce the effectiveness of contraceptives by affecting absorption.
Dr Kelechi urged women to seek proper medical guidance and avoid repeated or unprescribed use of emergency contraception, noting that misuse often delays proper STI treatment and compromises reproductive health.
She also highlighted Nigeria’s growing antibiotic resistance crisis, which is being fuelled by self-medication and poor regulation. The doctor called for nationwide awareness campaigns in schools, churches, and markets, alongside better training for patent medicine vendors to curb the spread of misinformation and unsafe drug practices.
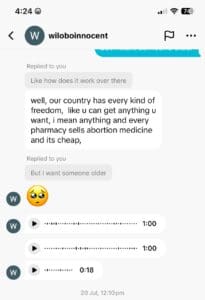
UGANDA’S CASE: FREEDOM OR DANGER?
The problem extends beyond Nigeria’s borders. In Uganda, pharmacist Wilobo Innocent describes a similarly dangerous culture of self-medication.
“Here, you can buy anything – abortion pills, tramadol, even morphine – no questions asked,” he says. “Girls get pregnant and just go buy pills to abort. It’s so easy now.
“But if used wrongly, the side effects are deadly. Some bleed to death. And if you use them too often, by the time you’re ready to have children, it may be too late.”
His fears mirror those of many across Africa that unrestricted drug access, compounded by misinformation, is quietly sabotaging the fertility and future of a generation.
WHAT MUST BE DONE
To stem this tide, Dr Chukwuneku urges three key interventions:
-
Expand Access to Correct Information: Public education campaigns via radio, TV, social media, and community groups must combat myths and promote safe contraceptive use.
- Improve Access to Regular Contraceptives: Women should not have to rely on emergency methods. Make long-term options affordable, accessible, and stigma-free.
- Enforce Antibiotic Control: Strict prescription-only enforcement, regular pharmacy inspections, and stiffer penalties are essential to reverse Nigeria’s antibiotic resistance trend.
“Emergency contraceptives are not abortifacients. They don’t cause infertility. And antibiotics do not prevent pregnancy,” Dr Chukwuneku concludes. “The danger lies in misuse and in silence. We must talk about it and act now.”
THE MYTHS THAT REFUSE TO DIE
| Myth | Fact |
|---|---|
| Ampiclox can prevent pregnancy | It cannot. It’s an antibiotic, not a contraceptive. |
| Emergency pills cause infertility | They don’t, but misuse can increase pregnancy risk. |
| You don’t need a prescription for antibiotics | You should. Self-medicating fuels drug resistance. |
Esther Ososanya is an investigative journalist with Pinnacle Daily, reporting across health, business, environment, metro, Fct and crime. Known for her bold, empathetic storytelling, she uncovers hidden truths, challenges broken systems, and gives voice to overlooked Nigerians. Her work drives national conversations and demands accountability one powerful story at a time.
- Esther OSOSANYA